Summary
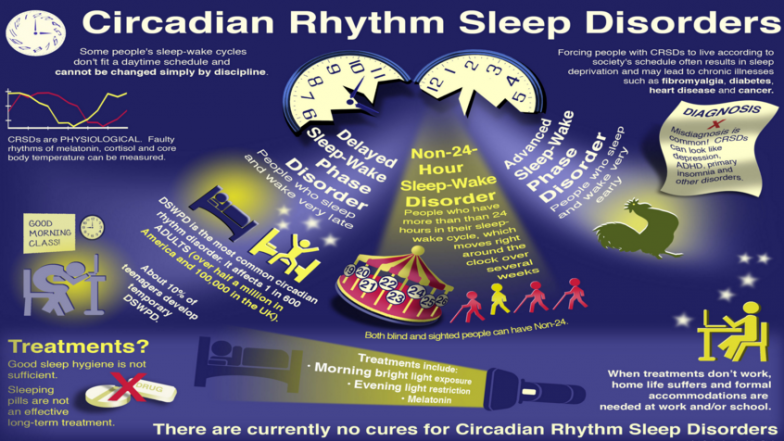
Circadian rhythm sleep disorders (CRSD), a family of sleep disorders, affect (among other bodily processes) the timing of sleep. People with circadian rhythm sleep disorders are unable to go to sleep and awaken at the times commonly required for work and school as well as social needs.
They are generally able to get enough sleep if allowed to sleep and wake at the times dictated by their “body clocks”. The quality of their sleep is usually normal unless they also have another sleep disorder.
OnAir Post: Circadian Rhythm Sleep Disorders